|
12/28/2023 0 Comments Severe upper middle abdominal pain This causes the pancreas to become inflamed.ĮRCP related pancreatitis. (The pancreatic duct delivers digestive enzymes from the pancreas to the small intestine.) When the pancreatic duct becomes blocked, enzymes can't flow properly. Gallstones that escape from the gallbladder can block the pancreatic duct. Alcohol combined with smoking increases the risk of acute pancreatitis. Alcohol use may be over a period of time or in a single binge. But certain people will develop pancreatitis after drinking large amounts of alcohol. 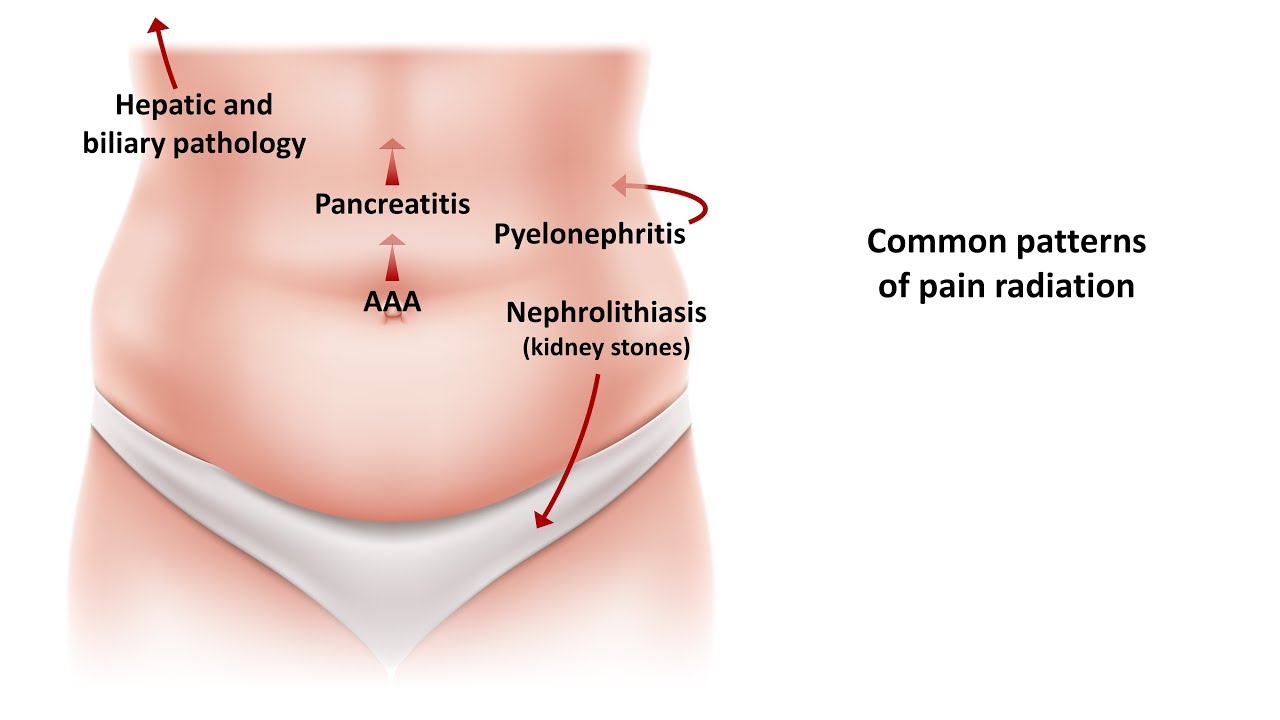
Post the medical procedure known as ERCPĪlcohol related pancreatitis. Most people who drink alcohol never develop pancreatitis.The most common causes of acute pancreatitis are: More enzymes are released into the surrounding tissues and bloodstream. 
In pancreatitis, enzymes that normally are released into the digestive tract begin to damage the pancreas itself. It produces digestive enzymes and hormones. The pancreas is located in the upper part of the abdomen, behind the stomach. Last updated on Apr 18, 2023.Īcute pancreatitis is a sudden inflammation of the pancreas. It is also important to review the past medical history such as comorbidities and medication use, especially opiate, nonsteroidal anti-inflammatory drugs (NSAIDs) as it can also aid in gauging the cause of the abdominal pain.Medically reviewed by. One should probe for coexisting symptoms such as nausea, vomiting, diarrhea, blood in stools and systemic symptoms such as fever or rash. Intermittent pain can have many causes but constant abdominal pain results only from a few gastrointestinal etiologies, such as chronic pancreatitis, malignancy, abscess, and psychiatric causes. Chronic abdominal pain is defined as a constant or intermittent pain occurring for >3 months while acute abdominal pain is when the pain has been occurring for up to several days subacute abdominal pain can span from several days up to 3 months. Typically, the pain caused by peptic ulcer disease, chronic mesenteric ischemia, or biliary and pancreatic pathologies worsens after the meal, while in IBS pain is relieved with bowel movements. constant) and the relationship to meals or bowel movements. It is also important to establish the duration and the pattern of the pain (intermittent vs. Lower abdominal pain arises from the colon (e.g., IBS and colitis), bladder, or reproductive organs. Mid-abdominal pain can be caused by the small bowel (e.g., Crohn’s disease, celiac disease, partial small bowel obstruction, and chronic mesenteric ischemia). Upper abdominal pain can arise from biliary, pancreatic, gastric, and duodenal pathology. The site and radiation of abdominal pain helps narrow down the differential diagnosis because the pain syndromes typically have characteristic locations. The abdominal pain characteristics, such as site, radiation, onset, the evolution of time, character, exacerbating/ameliorating factors, associations, and severity (SOCRATES ) can offer clues to the diagnosis (Table 2). The first step in managing a patient with chronic abdominal pain is to get a detailed history and the physical examination, even if these have a relatively low sensitivity and specificity in diagnosing the different causes of abdominal pain. Once a diagnosis of functional pain is established, repetitive testing is not recommended and the patient should be referred to receive psychological support (e.g., cognitive therapy) associated with available pharmacological therapeutic options. The functional disorders should be considered after the organic pathology has been confidently excluded. Key Messages: The primary role of the general practitioner is to differentiate an organic disease from a functional one, to refer to a specialist, or to provide treatment for the underlying cause of pain. 
This review will focus on the diagnostic tools which general practitioners utilize in the evaluation of chronic abdominal pain. 
Diagnostic investigations should be limited and adapted according to the clinical features, the alarm symptoms, and the symptom severity. Undiagnosed abdominal pain should be investigated starting with a detailed history and physical examination. A systematic approach for evaluating patients and initiating a management plan are recommended in the primary care setting. The costs associated with a diagnostic workup are an expensive burden to health care. In the absence of red flag features that herald more acute conditions, the majority of patients with chronic abdominal pain have a benign cause or a functional disorder (e.g., irritable bowel syndrome). Background and Summary: Chronic abdominal pain is a challenging complaint for both primary care providers and gastroenterologists alike, due to a broad differential diagnosis and sometimes extensive and negative workup. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
